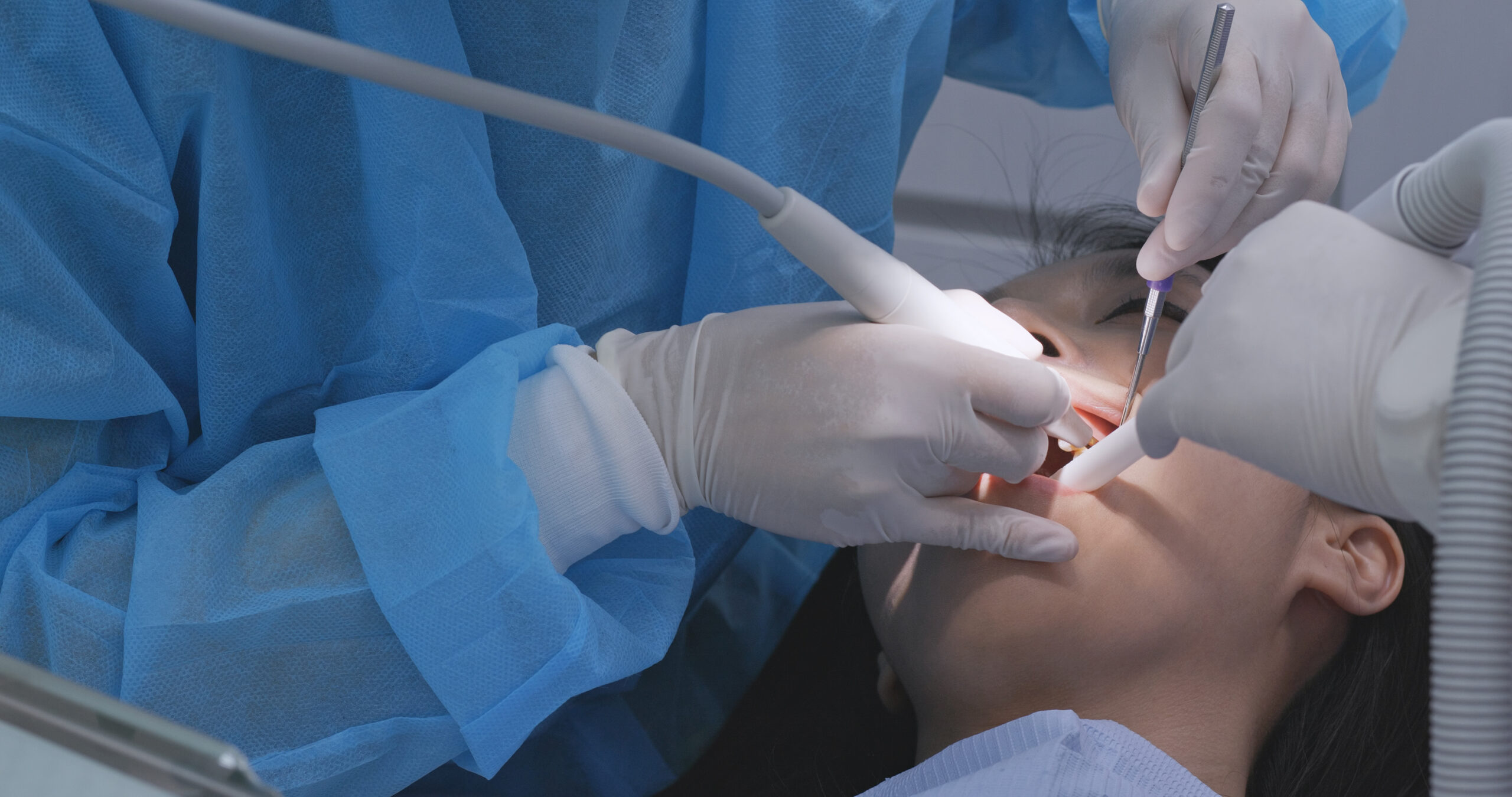
Biological Oral Surgery
Precision Surgery Guided by Biology, Healing & Long-Term Stability
At Nuffield Dental Jewel, Biological Oral Surgery refers to a surgical approach that prioritises tissue health, inflammation control, and predictable healing — rather than simply completing a procedure.
This philosophy applies to complex extractions, implant site preparation, jawbone surgery, and revision procedures where careful handling of bone and soft tissue is essential for long-term success.
What Is Biological Oral Surgery?
Biological Oral Surgery is an evidence-aligned surgical approach that focuses on:
- Meticulous removal of infected or inflamed tissue
- Preservation of healthy bone and gum structures
- Supporting natural re-vascularisation and healing
- Minimising surgical trauma where possible
- It is not an alternative form of dentistry. It is a refined way of performing oral surgery with greater respect for biology.
Biological Oral Surgery
When Biological Oral Surgery May Be Recommended
Biological oral surgery may be considered in situations such as:
- chronically infected or non-healing extraction sites
- preparation of bone prior to implant placement
- failed or compromised implant sites
- impacted or difficult tooth extractions
- jawbone conditions associated with persistent discomfort
- revision surgery following previous dental procedures
- Each recommendation is based on clinical findings, imaging, and patient-specific factors - not on routine or protocol-driven surgery.
Biological Oral Surgery & Implant Planning
Successful dental implants depend heavily on the quality of the surrounding bone and gum tissue. Biological oral surgery is often integrated into implant treatment to:
- prepare compromised sites
- manage residual infection or inflammation
- preserve bone for optimal implant stability
- reduce the risk of future complications
- Whether implants are placed immediately or in a staged manner depends on biology, anatomy, and healing capacity - all of which are carefully assessed.

Nuffield Dental Jewel
Conditions Often Evaluated as Part of Surgery
As part of our biological surgical assessment, we may evaluate for:
- chronic inflammatory bone changes
- persistent post-extraction discomfort
- localised jawbone pathology
- atypical facial or jaw pain where dental causes are suspected
- Not all findings require surgery. Conservative management is always considered first.
What Our Surgical Approach Involves
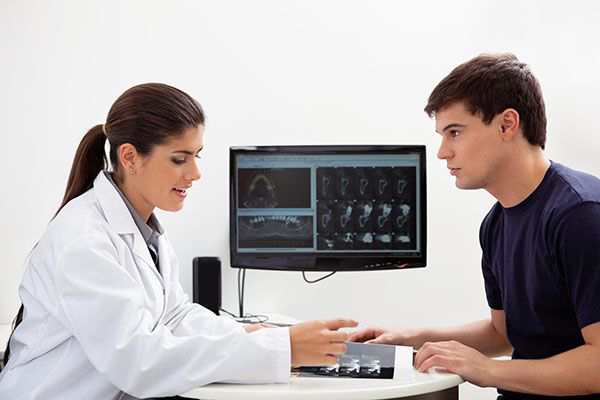
Careful Assessment & Imaging
Before any surgery, we perform a detailed evaluation that may include:
- comprehensive clinical examination
- 3D CBCT imaging to assess bone anatomy and surrounding structures
- review of medical history and healing risk factors
- This allows us to plan surgery with accuracy and foresight.
Thorough Site Preparation
During surgery, emphasis is placed on:
- careful debridement of inflamed or non-vital tissue
- removal of infected granulation tissue when present
- preservation of healthy surrounding bone
- maintaining stable soft-tissue margins
- Our goal is to create a clean, biologically favourable environment for healing or future restoration.

Regenerative Support (When Indicated)
In selected cases, regenerative adjuncts such as PRF (Platelet-Rich Fibrin) may be used to:
- support soft-tissue healing
- encourage early bone remodelling
- reduce post-operative inflammation
- These are adjuncts, not substitutes for good surgical technique, and are recommended selectively based on clinical need.

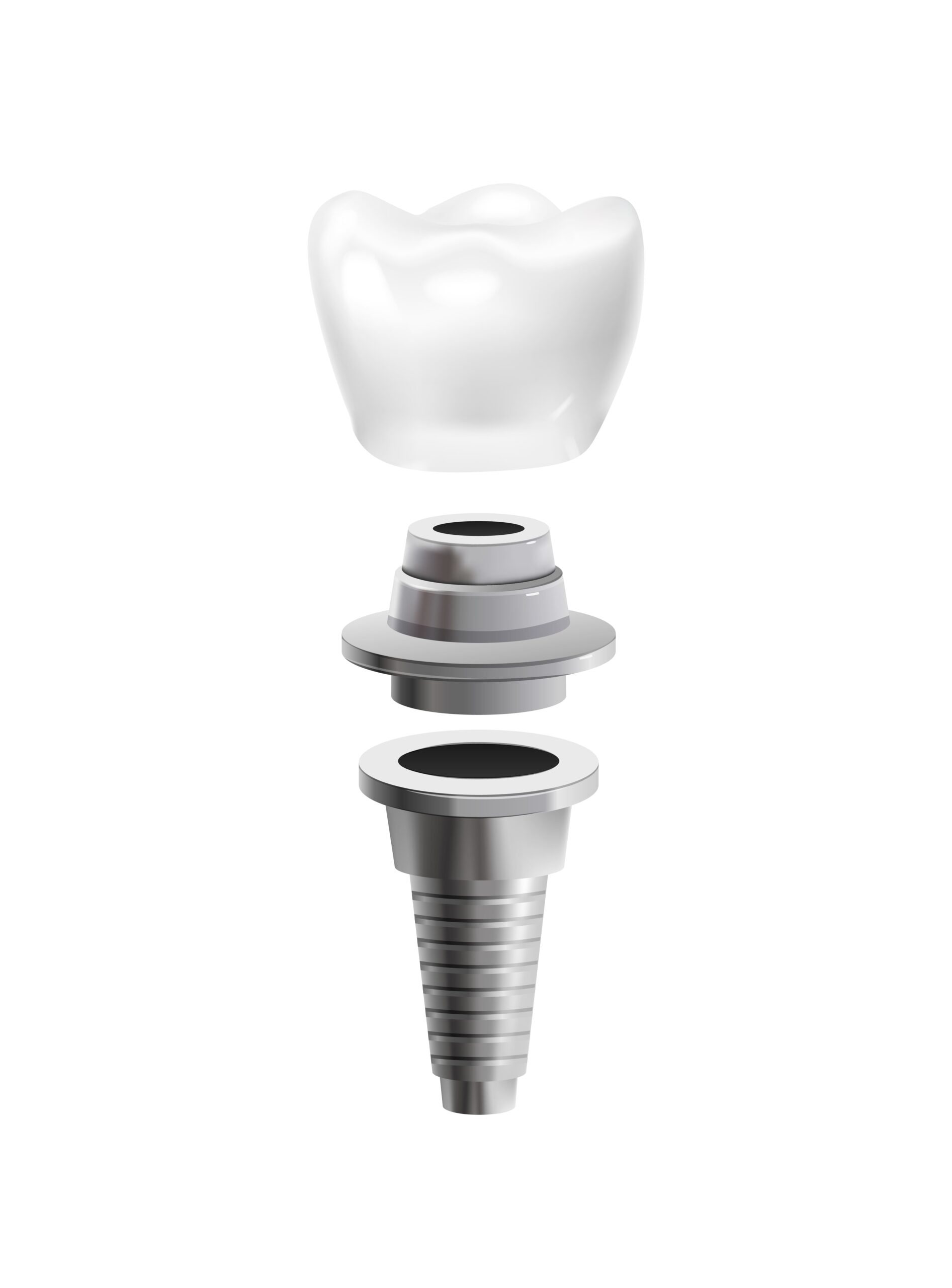
Durability and Strength
Contemporary ceramic implants are made to withstand functional bite forces and long-term use when placed with correct surgical technique and restorative planning. (PMC)
- Full medical and dental history
- 3D imaging (CBCT) to assess bone anatomy
- Gum health and bite analysis
The Ceramic Implant Process at Nuffield Dental Jewel
Our ceramic implant workflow emphasises safety, clarity, and comfort:
Comprehensive Assessment
We begin with a detailed evaluation including:
- Full medical and dental history
- 3D imaging (CBCT) to assess bone anatomy
- Gum health and bite analysis
We explain each stage in detail, including aftercare and maintenance.
Individualised Planning
Every implant plan considers your tissue biology, smile aesthetics, and long-term functional goals.
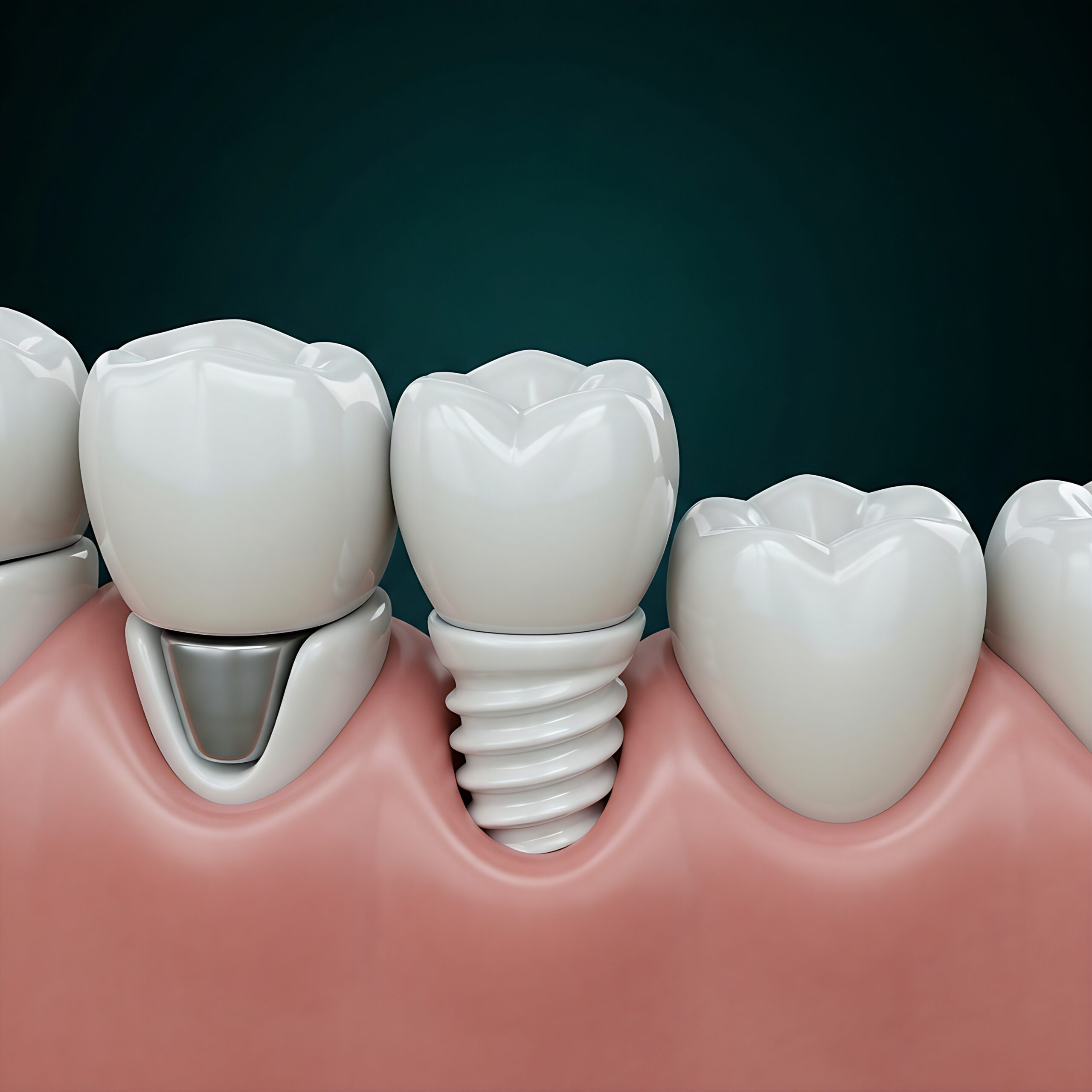
Surgical Placement
Ceramic implants are placed with precise surgical technique and digital guidance where appropriate. Regenerative support such as PRF may be recommended when indicated to support healing and tissue integration.
Restoration
After integration and healing, custom crowns or bridges are placed to restore function and aesthetics.

What Biological Oral Surgery Is Not
To be clear, our approach:
- Does not promise systemic disease treatment
- Does not rely on speculative diagnoses
- Does not replace medical care
- Does not involve unnecessary surgery
- Our focus is local tissue health, function, and predictability.
dental implants
Healing, Recovery & Follow-Up
After biological oral surgery, patients are supported with:
- clear post-operative instructions
- tailored pain and swelling management
- review appointments to monitor healing
- planning for subsequent restorative phases if needed
- Healing timelines vary depending on the extent of surgery and individual biological factors, which are discussed in advance.
Nuffield Dental Jewel
How Biological Oral Surgery Fits Into Your Overall Care
Biological oral surgery is rarely a standalone treatment. It is usually part of a broader care pathway that may include:
- ceramic or titanium dental implants
- regenerative support
- restorative or aesthetic dentistry
- long-term maintenance planning
- We ensure all stages are coordinated and sequenced logically.
Why Patients Choose Nuffield Dental Jewel
Patients seeking biological oral surgery value:
- Clear explanations and transparency
- Clear explanations and transparency
- Respect for healing biology
- Long-term stability over speed
Every recommendation is made with your best interests and long-term outcomes in mind.